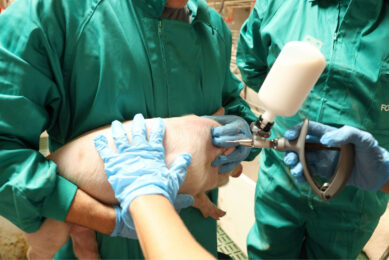
How to further improve M. hyo vaccine efficacy?
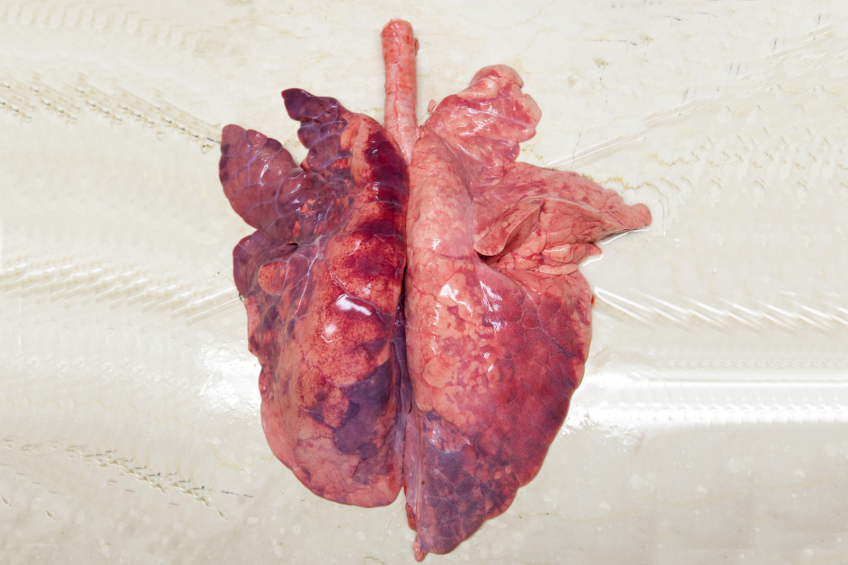
Although immunity against M. hyo is not fully understood, it is a fact that vaccination helps reduce the size and duration of lung lesions. Both antigenic and adjuvant components are essential to generate immune responses. Lipopolysaccharides appear to boost both humoral and cell-mediated responses to an M. hyo vaccine.
Mycoplasma hyopneumoniae (M. hyo) is a primary pathogen causing Enzootic Pneumonia (EP), one of the most prevalent respiratory diseases in pigs. It is also one of the main pathogens involved in the Porcine Respiratory Disease Complex (PRDC). EP and PRDC cause substantial economic losses in the swine industry due to decreased growth rate, increased feed conversion ratio, increased treatment costs and in the case of complicated PRDC, also increased mortality.
M. hyopneumoniae was found to facilitate the replication of PRRSv and PCV2, as well as to potentiate the severity of pneumonia in pigs due to PRRSv or A. pleuropneumoniae.
Role of immunity
Immunity against M. hyopneumoniae is not fully understood. The fact that the pathogen is non-invasive and can induce pneumonia, implies a significant role of strong immune response. M. hyo interacts with almost every component of the host immune system. An increase in pro- and anti-inflammatory, and immunoregulatory mediators such as prostaglandin E2 (PGE2), various interleukins, tumor necrosis factor-alfa (TNF-α) and interferon-gamma (IFN-γ) have been demonstrated in infected lungs. Some of those contribute to the clearance of the pathogen; others on the contrary, play the role in the suppression of the efficacy of the immune system.
What can vaccination do to help pigs?
As of today, vaccination does not prevent colonisation of pigs by M. hyo when they are in contact with the infected animals. However, the lung lesions in vaccinated pigs are smaller and heal sooner than in the non-vaccinated animals, which also excrete more M. hyo in the upper respiratory airways. This suggests that vaccinated pigs develop less or fewer lesions in the lungs, the multiplication of M. hyo is reduced and excretion via nasal route is also reduced. The major advantages of vaccination include the improvement in daily weight gain (2-8%) and feed conversion ratio (2-5%).
There are multiple mechanisms of the immune responses involved in the protection against M. hyo. Vaccinated pigs subsequently infected with M. hyo had significant changes in the pulmonary immune system compared to non-vaccinated controls. Both mucosal antibodies and cellular immune response seem important for the control of mycoplasmal pneumonia. The numbers of macrophages, neutrophils and lymphocytes were significantly lower in BAL fluid in vaccinated pigs, while there was an increased amount of IgA bearing cells in the lungs. Vaccination increases both IgA and IgG presence in the lungs after the infection. The IgA antibody prevents mycoplasmal adherence onto the respiratory tract while IgG is involved in antigen opsonisation and enhances phagocytosis by alveolar macrophages. Decrease of the TNF- α, IL-1 and IL-6 production in vaccinated animals may lead to the suppression of inflammatory cell infiltration resulting in fewer lung lesions.
Activation via pattern-recognition receptors
After the infection as well as after vaccination, one of the first events in the reaction of the host is the interaction between the foreign antigen and professional antigen presenting cells (APCs). They are crucial in triggering the innate response and in initiating adaptive immunity by the presentation of processed antigens to T-lymphocytes, supported by various co-stimulatory proteins and the production of cytokines. To direct these functions during an immune response, monocytes or other APCs become activated through binding of conserved microbial structures to their respective pattern-recognition receptors (PRRs). Within the group of PRRs, Toll like receptors (TLRs) play a well-known role in the initiation of such immune responses. Toll-like receptors recognise a variety of components such as lipopolysaccharides, lipoproteins and other bacterial components.
Figure 1 – Cascade of signals activating Th1 and TH2 responses after vaccination.

Surface lipoproteins in mycoplasmas have a strong immunomodulatory potency, especially for activating macrophages. Lipoproteins interact with toll-like receptors (TLR). M. hyo is known to stimulate macrophages through the binding to TLR 2 and TLR 6.
TLR4 mediates signalling by bacterial lipopolysaccharides (LPS). LPS-induced TLR-4 signalling belongs to the key innate mechanisms of immune responses which also trigger the subsequent activation of adaptive immunity. LPS have been shown to initiate multiple intracellular signalling events, including the activation of NF-κB, which leads to the synthesis and release of a number of pro-inflammatory mediators, including interleukins IL-1, IL-6, IL-8, and TNF-α. The interaction between TLR4-mediated and other signalling cascades results in the effective immune response.
Figure 2 – In vitro test measuring the oxidative burst of the peripheral blood monocytes after the exposure to J5 (FA 12/22). All monocytes (100%) were activated.

Experimental studies
Several experimental studies have demonstrated good protection induced by Hyogen (Ceva Animal Health), an inactivated M. hyo vaccine adjuvanted by a special adjuvant named Imuvant. The systemic immune reaction as well as modulation of the local immune responses namely strong IgA response and lower production of pro-inflammatory cytokines, lower M. hyo load in the excretions and significant reduction of lung lesions were described. Besides the unique M. hyo strain used in the vaccine, the adjuvant plays a significant role in its efficacy.
The adjuvant, developed by Ceva, consists of an optimised formulation of non-toxic LPS derived from Escherichia coli J5 in an oil-in-water emulsion. Lipopolysaccharides stimulate the innate immune response, via activation of macrophages and other antigen presenting cells. The lipoprotein antigens from M. hyo bind to the aqueous/oil interface, which increases the uptake by the APCs. The cascade stimulation of various compartments of the immune system leads to robust antibody- and cell-mediated immune responses. The result is an efficient prime of antigen recognition and active immune response, long immunological memory and therefore a more complete protection against M. hyo.
In the in vitro studies J5 LPS stimulated intensively the activity of monocytes, which was measured by the oxidative burst (see Figure 1). The release of reactive oxygen (oxidative burst) is used as an indicator of activation of leukocytes.
Figure 3 – M. hyo specific serological response 21 days after vaccination measured by M. hyo ELISA in the log scale.

J5 component
A recent study assessed the boosting effect of the adjuvant’s J5 component on the vaccine’s efficacy in piglets. Pigs were either vaccinated with the vaccine containing the full adjuvant including J5 LPS or with a test vaccine containing the M. hyo antigen adjuvanted only with the mineral oil but not the J5. The non-vaccinated pigs served as a positive control. Eighteen days after vaccination, the pigs were challenged with a virulent M. hyo strain. At 28 days post challenge the animals were slaughtered and subjected to lung scoring.
The results demonstrated stronger humoral and particularly cell-mediated immune responses to the vaccine containing J5 compared to the test vaccine without J5.
The evaluation of lung lesion scoring in the euthanised pigs demonstrated a significant reduction of bronchopneumonia in pigs vaccinated with the vaccine and J5-adjuvant compared to the non-vaccinated control (p<0.05) and also numerical reduction of the lesions with vaccinated pigs compared to animals vaccinated with the test vaccine without j5 (>Figure 4).
Figure 4 – Cell-mediated response measured 21 days post-vaccination by IFN M. hyo specific Elispot in the log scale.

Conclusion
These studies confirm a beneficial influence of J5 in potentiating the adjuvant role of Imuvant in inducing strongly efficient immune responses and protection against the development of bronchopneumonia after M. hyo infection. Especially the cell-mediated immunity was significantly stronger due to J5 together with higher antibody production. Boosted immunity resulted in lower lung lesion scores. The adjuvant supports the M. hyo antigens in Hyogen to make it an efficient solution in the still problematic control of enzootic pneumonia.
Figure 5 – Mean weighted lung scores measured in pigs 28 days post-challenge with the virulent M. hyo strain. Pigs were vaccinated with Hyogen (containing J5) or with the test vaccine without J5 or with placebo.

References available on request.