Pig heart transplanted into American man
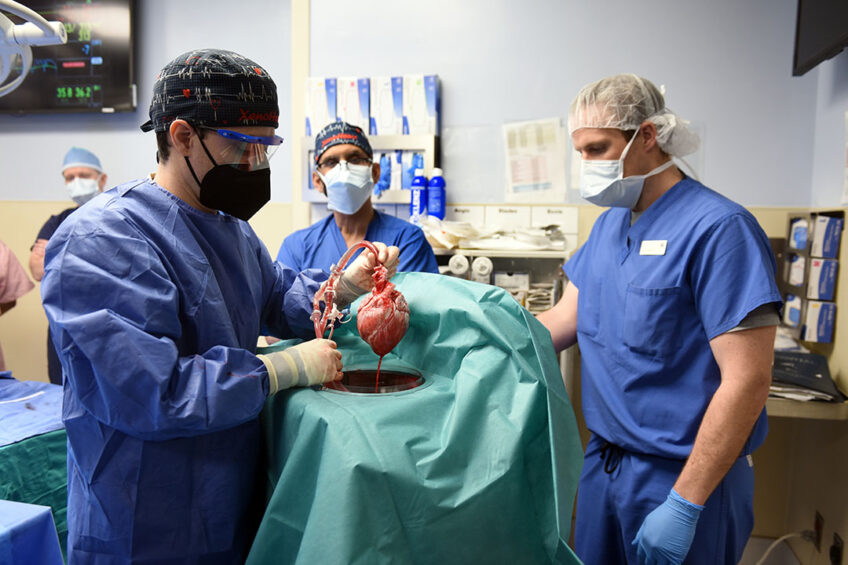
For the first time, a (genetically modified) pig heart is implanted into a human. A man from the United States with terminal heart disease was received the heart – and 3 days later he was doing well, according to the medical team.
A team at the University of Maryland performed the surgery. It demonstrated the feasibility of a pig-to-human heart transplant, a field made possible by new gene editing tools, according to a news article on the university’s website. If proven successful, scientists hope pig organs could help alleviate shortages of donor organs. For patient David Bennett (aged 57), the heart transplant was his last option.
Permission to move ahead with pig heart transplant
To move ahead with the experimental surgery, the university obtained an emergency authorisation from the US Food and Drug Administration (FDA) through its compassionate use programme.
Revivicor, a regenerative medicine company based in Blacksburg, VA, provided the genetically-modified pig to the xenotransplantation laboratory at the University of Maryland. On the morning of the transplant surgery, the surgical team removed the pig’s heart and placed it in a machine that keeps the heart preserved until surgery.
Pigs are a potential source of transplants because their organs are relatively similar to humans. Other organs from pigs being researched for transplantation into humans include kidneys, liver and lungs.
Making the pig heart suitable for surgery
Earlier efforts at pig-to-human transplants often failed because of genetic differences that caused organ rejection or viruses that posed an infection risk. Gene editing solved that issue. In the heart implanted in Bennett, 3 genes previously linked with organ rejection were “knocked out” of the donor pig, and 6 human genes linked with immune acceptance were inserted into the pig genome.
Researchers also deleted a pig gene to prevent excessive growth of the pig heart tissue.
The physician-scientists also used a new drug along with conventional anti-rejection drugs, which are designed to suppress the immune system and prevent the body from rejecting the foreign organ. The new drug used is an experimental compound made by Kiniksa Pharmaceuticals.











